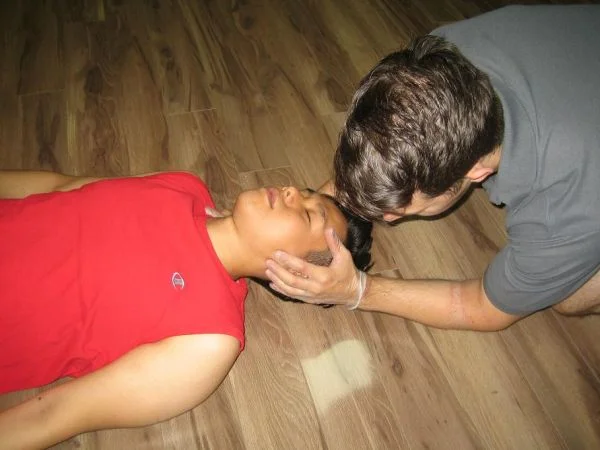
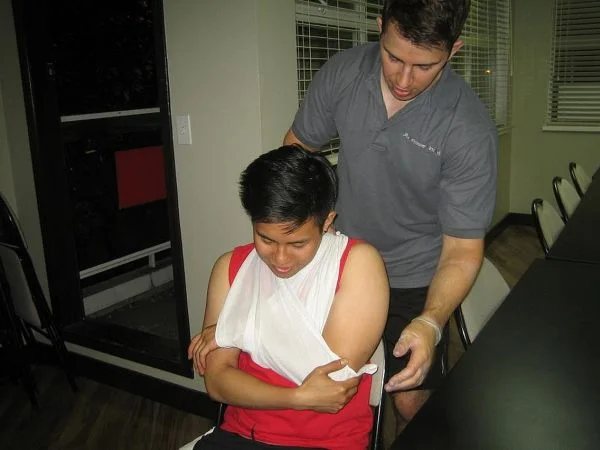
Standard First Aid Training
This two day, comprehensive first aid course is recognized by government, academic, workplace and legislative standards. This course includes training in CPR and AED and provides certification that is valid for 3 years throughout Canada.
Recertifications Classes
Whether you need to re-certify first aid and CPR or you only need to recertify your CPR certificate we have a class for you. We offer workplace approved recertification programs multiple times throughout the week. We proudly offer the lowest prices and provide the most experienced teachers.
CPR and AED Courses
Individuals that need to be certified in CPR level “A” , “C” or “HCP” and do not need certification in first aid can take a workplace approved CPR course. These courses include certification in the use of automated external defibrillators. Certificates are valid for 3 years except for CPR HCP which certificate is valid for 1 year.
Standard Childcare First Aid Courses
Participants that need to be certified to work in the childcare industry should take workplace approved standard childcare first aid courses. This two day course includes training in various first aid components as well as CPR level “B” and on how to use an automated external defibrillator (AED).
Mask Fit Testing
At Regina First Aid we offer Mask Fit Testing for individuals looking for qualitative tests to determine whether the mask used in the workplace, school or lab provides effective protection. This 15 minute test is offered multiple times per week and provides candidates with the training to properly care, maintain and put on a mask.
3M Masks for Sale
Do you need 3M Masks for your workplace? Visit our mask sales page to view the various masks that we have for sale that meet CE and FDA standards. We are a authorized sales provider of these masks and we can provide almost any quantity of masks. Free shipping and handling throughout Canada. Click here for more information about our masks or to purchase.
Welcome To St Mark James Training – Regina First Aid
Do you need to speak someone about registering for a course or have questions about what we offer? Not only can you give us a call at 306-988-4432, but we offer a call-back option where we can contact you at your request.
We offer a number of ways for you to contact us. We also offer private training at your facility or ours. To contact us via telephone, email or contact form click the following button
We proudly offer a wide range of courses at the lowest prices in Regina. Check out our course price / list by clicking the button below
Need help finding a course? You can check out all of our upcoming courses by clicking the following link
Regina First Aid is committed to offering you the largest variety, highest quality and lowest priced workplace approved first aid and CPR courses. We are experienced providers that offer courses throughout Canada and are dedicated to offering you the very best. First aid and CPR training has been synonymous with mundane and boring lectures so we are determined to offer educational, interactive, comfortable and entertaining courses. All first aid and CPR classes include training and certification in the use of automated external defibrillators (AED). All of our first aid and CPR courses are offered through the provincially approved providers and when candidates successfully complete the course they will receive certificates that are nationally accredited and meet workplace and academic requirements / standards.
Regina First Aid Courses
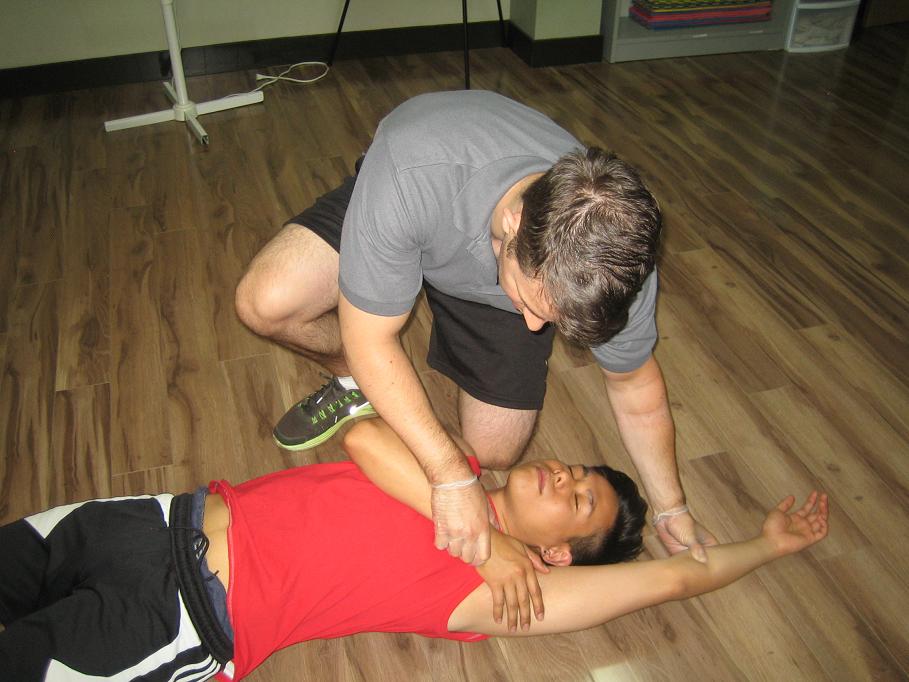
Standard / Intermediate First Aid Courses
Regina First Aid proudly offers provincially recognized standard first aid courses. This course, also referred to as intermediate first aid, includes training and certification in cardiopulmonary resuscitation (CPR) and in the use of automated external defibrillators (AED).
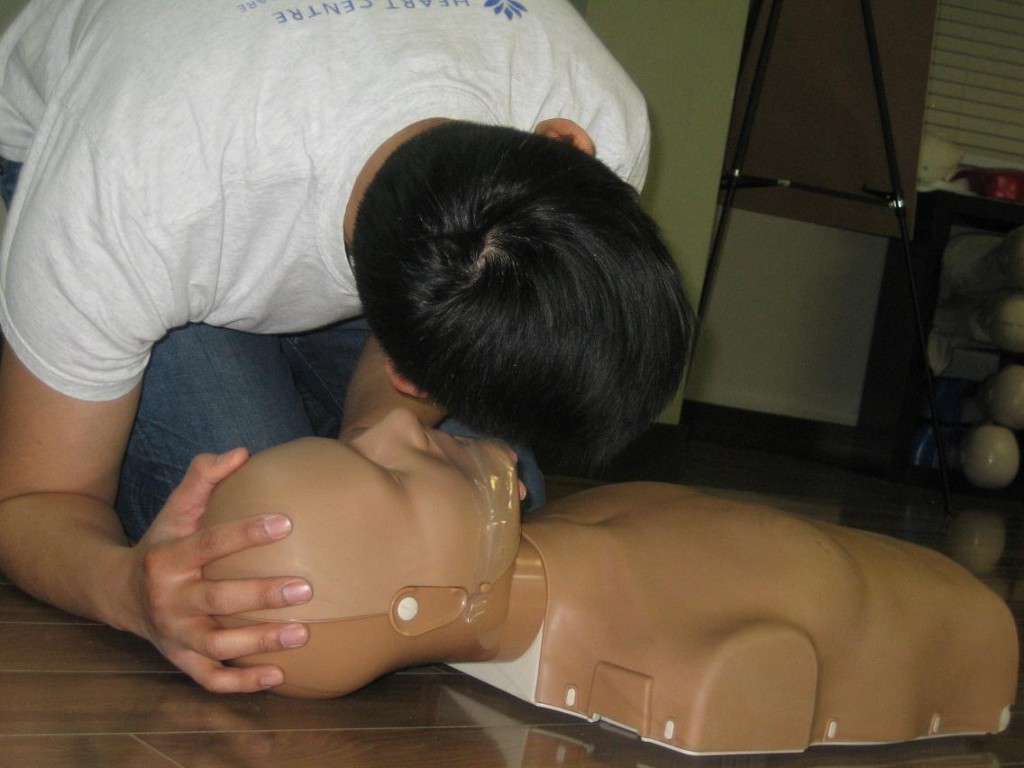
Emergency First Aid Courses
Regina First Aid proudly offers emergency first aid courses. This Saskatchewan recognized certification class, also referred to as basic first aid includes training and certification in cardiopulmonary resuscitation (CPR) and in the use of automated external defibrillators (AED).
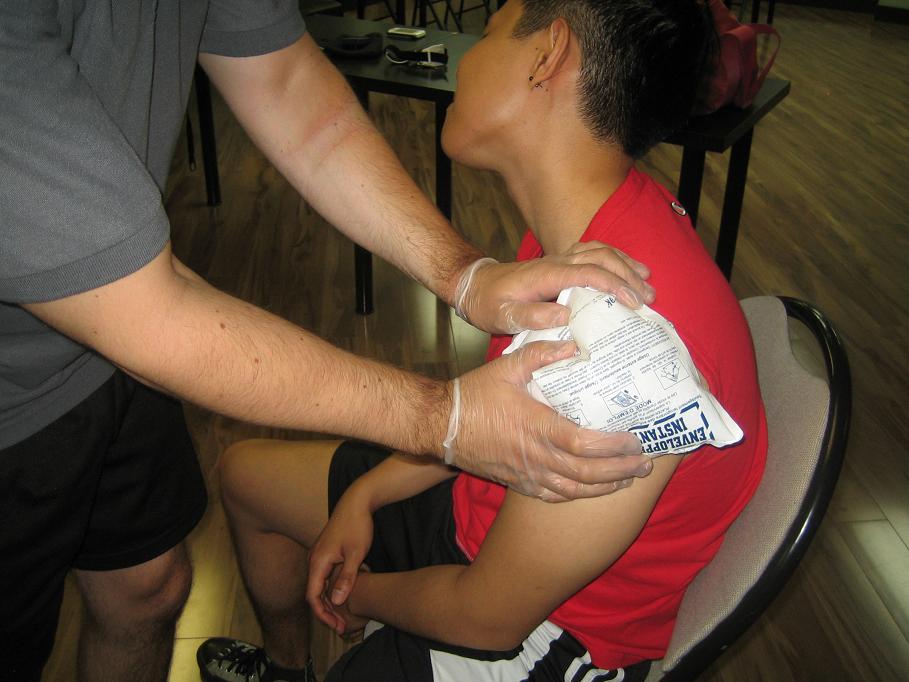
Standard Childcare First Aid Courses
Regina First Aid proudly offers standard child care first aid and CPR level “B” courses. This course is designed for candidates that work or want to work in the child care industry. This is one of the most extensive first aid and CPR courses available.
CPR Courses

CPR level “A” Course
Regina First Aid proudly offers cardiopulmonary resuscitation (CPR) level “A” courses. This course is the most basic CPR course offered with us. Candidates will learn basic CPR techniques for adult rescues. Upon completion of the course successful students will receive a CPR and AED certificate that meets many workplace and academic requirements and is valid for 3 years.

CPR level “C” Course
Regina First Aid proudly offers workplace and academic approved CPR level “C” training. This course is one of the most popular stand-alone CPR courses available. No first aid certification is included in this 5 hour course. This course is designed for candidates that require only cardiopulmonary resuscitation (CPR) and automated external defibrillator (AED) training.

CPR HCP Course
CPR level “C” for health care providers, also known as CPR “HCP”, is the most comprehensive level of CPR training available to our participants. This CPR and AED course teaches participants CPR rescue skills for victims of all ages. Participants will also learn to used advanced equipment and learn how to provide CPR with trained assistance.
Recertifications
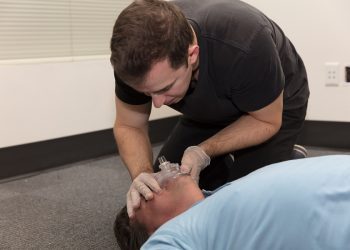
Standard / Intermediate First Aid Recertification
Regina First Aid proudly offers provincially recognized standard / intermediate first aid and CPR recertification courses. This class is designed for individuals with current standard first aid awards that need to renew certification prior to expiry. This course takes 8 hours to complete and costs 94.99. CPR and AED certification and training is also included in this course. Participants can select either CPR level “C” or “HCP” to partner with the recertification course.

Standard Childcare First Aid Recertification
We proudly offer standard childcare first aid recertifications for individuals that are looking to renew expiring childcare first aid awards. This 8 hour course includes CPR level “C” certification and automated external defibrillator (AED) training. Participants in this course will review all of the components from the original standard childcare first aid in a condensed format.
Here is a List of Our Next 60 Courses:
| Event | Venue | Spaces Remaining | Date | |
|---|---|---|---|---|
| Standard Childcare First Aid and CPR B Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
2 |
|
Register |
| Standard First Aid and CPR Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
9 |
|
Register |
| First Aid and CPR Re-Certification in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
3 |
|
Register |
| Mask Fit Testing | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
4 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
2 |
|
Register |
| Emergency childcare first aid And CPR B | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
5 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) and CPR HCP Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
5 |
|
Register |
| Standard Childcare First Aid and CPR B Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
3 |
|
Register |
| Standard First Aid and CPR Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
12 |
|
Register |
| First Aid and CPR Re-Certification in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
5 |
|
Register |
| Mask Fit Testing | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
7 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
2 |
|
Register |
| Emergency childcare first aid And CPR B | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
5 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) and CPR HCP Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
3 |
|
Register |
| Standard Childcare First Aid and CPR B Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
2 |
|
Register |
| Standard First Aid and CPR Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
9 |
|
Register |
| First Aid and CPR Re-Certification in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
5 |
|
Register |
| Mask Fit Testing | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
8 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
4 |
|
Register |
| Emergency childcare first aid And CPR B | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
5 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) and CPR HCP Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
3 |
|
Register |
| Standard Childcare First Aid and CPR B Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
3 |
|
Register |
| Standard First Aid and CPR Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
13 |
|
Register |
| First Aid and CPR Re-Certification in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
5 |
|
Register |
| Mask Fit Testing | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
10 |
|
Register |
| Basic Life Support (BLS) / CPR and AED Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H1 |
7 |
|
Register |
| Emergency childcare first aid And CPR B | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
5 |
|
Register |
| Emergency First Aid with Basic Life Support (BLS) and CPR HCP Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
3 |
|
Register |
| Standard Childcare First Aid and CPR B Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada |
3 |
|
Register |
| Standard First Aid and CPR Course in Regina | 3426 Saskatchewan Drive Regina Saskatchewan Canada S4T 1H7 |
14 |
|
Register |
What Our Students Say About Us!

 Juhee Hwang (Jayde)I showed up in the building for my recertification and this education experience was more than what I came to expect. Full demo of each scenarios and thorough procedure explanation really helped. Good instructor, good system.
Juhee Hwang (Jayde)I showed up in the building for my recertification and this education experience was more than what I came to expect. Full demo of each scenarios and thorough procedure explanation really helped. Good instructor, good system. Gregory EzeobiI was provided a nice and detailed explanation of the standard first aid procedure and it didn't feel long because they taught so well. Would definitely recommend
Gregory EzeobiI was provided a nice and detailed explanation of the standard first aid procedure and it didn't feel long because they taught so well. Would definitely recommend Akintunde StephanieErin and David were nice and they made the class worthwhile. A really nice place
Akintunde StephanieErin and David were nice and they made the class worthwhile. A really nice place Andy SinnettThis course was great, 10/10 for sure. I’ve taken first aid before and it was just reading from a book and practicing things on a partner. This course had videos and an instructor that actually seemed to care and teach us the relevant things we really need to know. Bonus, no having to practice on another person which is kind of nice they have dummy’s for that. The class size was also smaller so it was easier to ask questions and less distractions. Erin the instructor was very friendly, very knowledgeable on first aid and didn’t just sit there reading from a manual. I will definitely be going back here for recertification when I need it 🙂
Andy SinnettThis course was great, 10/10 for sure. I’ve taken first aid before and it was just reading from a book and practicing things on a partner. This course had videos and an instructor that actually seemed to care and teach us the relevant things we really need to know. Bonus, no having to practice on another person which is kind of nice they have dummy’s for that. The class size was also smaller so it was easier to ask questions and less distractions. Erin the instructor was very friendly, very knowledgeable on first aid and didn’t just sit there reading from a manual. I will definitely be going back here for recertification when I need it 🙂 Eva RicciI reviewed and got a keychain! Excellent service
Eva RicciI reviewed and got a keychain! Excellent service Ava StouseStories are detailed and engaging, videos are extremely helpful and the instructor adds useful information.
Ava StouseStories are detailed and engaging, videos are extremely helpful and the instructor adds useful information.
Serving Regina and the surrounding areas in Saskatchewan with the lowest priced government approved first aid and CPR courses since 2013.